 
The surgical approach mostly used in humeral fractures is open reduction and internal fixation (ORIF) with plate, but considering the comminution and the risk of non-union in our patient, this method was not applicable. Therefore, we chose a fixation strategy for the management of this patient. Being considered as a relative indication, fixation is recommended in both comminuted and open fractures. Arthroplasty is an alternative treatment option for 3-parted and displaced anatomical neck fracture, but regarding to the patient’s age and massive soft tissue defect, we preferred to try an osteosynthesis method first. However, a small limitation of abduction and forward flexion in terminal ROM were detected and the assessed disabilities of the arm, shoulder and hand (DASH) score was10.Īccording to the available literature, several options have been introduced for humeral fractures including, closed reduction and splinting, closed reduction and intramedullary nailing (both rigid and elastic), open reduction and internal fixation with various plates, minimally invasive percutaneous plate osteosynthesis (MIPPO), and external fixation and arthroplasty. 
4.), with no signs of infection and full elbow ROM. At the end of the 7th month of the follow-up period, complete union of the fracture was achieved (Fig. Thereafter physiotherapy for patient was done for 20 sessions. After 6 months, a near total union was observed in X-ray therefore, all screws and TENs were removed. Thereafter, the brace was discontinued and passive pendulum shoulder exercise commenced (Figs. A partial union (consolidation) was found on the X-ray unexpectedly, and considering the presence of comminution and fixation with elastic nails which is a non-rigid fixation, we continued the splint until the partial union was achieved and then removed it so that the patient could go through the recovery period with less discomfort. Two months after the trauma, full elbow range of motion (ROM) was achieved. Splint was replaced with Sarmiento brace and the elbow movements were initiated. After 5 days, patient was discharged with necessary post-operative instructions after graft site healing assurance.Īfter 20 days while full healing of the donor and graft sites were achieved, the sutures and splint were removed. Following the confirmation of absence of any infection and growth of the granulation tissue, patient was readmitted for skin graft. The patient was discharged and advised to use a 10-day vacuum dressing. The post-operative neurovascular tests were normal. Two titanium elastic nail (TEN) were inserted with rotational forces and anchored to the subchondral bone since the humeral head had a fracture. Afterwards, two small incisions were made over both epicondyles of humerus, and after awl insertion, fluoroscopic guided closed reduction of humerus was achieved by longitudinal traction, external rotation, and abduction. Through a deltopectoral approach, reduction of greater tubercle, anatomical neck and head-split component (about 20% of head) attained and were fixed by 3 screws. First, the wound was irrigated with low pressure pulsatile manner with more than 6 L of normal saline serum, followed by the debridement of the unviable tissues. Surgery was performed in semi-sitting position on the following day. To the best of our knowledge, no similar patient with such complex injuries has been described and treated with this approach in the literature, and the reported case and treatment approach in this study could help future cases and surgeons to achieve successful outcomes. In this study, we reported a patient with multifocal comminuted open fracture of humerus with severe soft tissue defect who was treated with and innovative approach using elastic medullary nailing and skin grafting to repair the humerus and soft tissue injury. 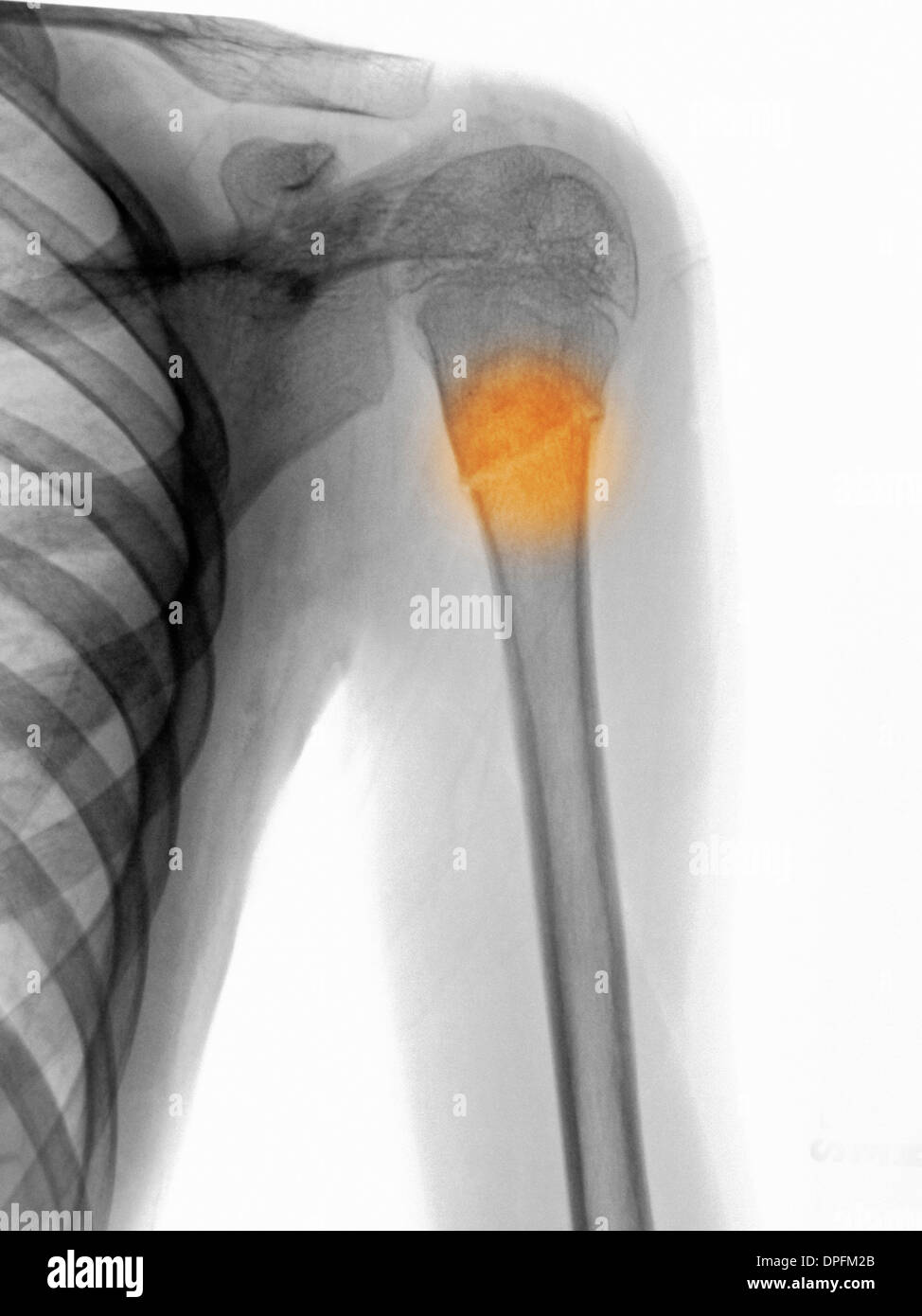
Choosing the best treatment strategy for a multifocal comminuted open fracture of humerus associated with severe soft tissue defect and articular involvement is challenging, which could come up for every orthopedic surgeon specially for those working in trauma centers. Concomitance of severe soft tissue defect requiring soft tissue reconstruction with aforementioned injuries is scarce in literature. Coincidence of highly comminuted proximal and diaphyseal fracture makes these conditions even more complicated and challenging. In addition, head-split and anatomical neck humeral fractures are extremely rare. Ipsilateral multifocal humeral fracture is an infrequent injury. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
